Benzodiazepine Addiction: Definition, Signs and Symptoms, Effects, Types, Withdrawal, Treatment

Benzodiazepine addiction is the misuse of benzodiazepines in any way not directed by a doctor, leading to dependence and harmful consequences. Benzodiazepines are prescribed for anxiety, insomnia, and seizures, but misuse includes taking higher doses, using without a prescription, or combining with other substances. In the United States, 5.3 million adults (2.2%) reported misusing benzodiazepines, […]
Hashish (Hash) Addiction: Signs, Causes, Dangers, Withdrawal Risks, Treatment, and Prevention

Hashish addiction represents a growing concern worldwide, particularly due to its potent psychoactive properties. Approximately 147 million people, accounting for 2.5% of the global population, use cannabis annually, compared to 0.2% who use cocaine and another 0.2% who consume opiates, according to the World Health Organization (WHO). The signs of hashish addiction include intense cravings, […]
Gabapentin Addiction: Symptoms, Effects, Treatment, and Prevention

Gabapentin addiction develops when repeated use of the medication alters brain chemistry, leading to compulsive consumption beyond prescribed doses. Gabapentin, a prescription medication marketed under the brand name Neurontin, is used to manage nerve pain, seizures, and other chronic conditions. While intended for therapeutic purposes, its misuse or excessive consumption precipitates dependency, resulting in gabapentin […]
Antihistamine Addiction: Symptoms, Effects, Withdrawal, and Treatment
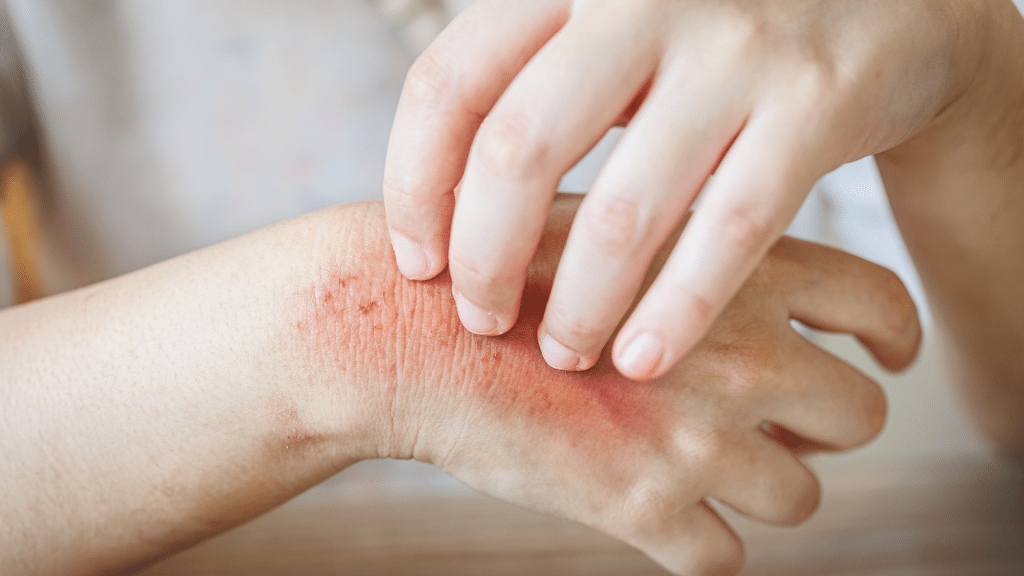
Antihistamine addiction is an increasingly recognized dependency on allergy medications, characterized by physical and psychological symptoms resulting from habitual overuse. Although antihistamines are prescribed for allergy relief, some individuals consume them excessively, seeking their sedative effects. Common antihistamines that are abused are diphenhydramine (found in Benadryl), promethazine, hydroxyzine, and chlorpheniramine. According to Dinwiddie, G.’s 2022 […]
14 Signs Of Liver Damage Caused By Alcohol and Cirrhosis

Alcoholic liver disease refers to liver damage that results from long-term heavy alcohol use. This condition, also known as ALD, progresses through different stages, from fatty liver to alcoholic hepatitis and eventually cirrhosis. Alcoholic liver disease (ALD) represents a spectrum of liver conditions as the primary stages of ALD include steatotic (fatty) liver, acute hepatitis, […]
Meth Detox: Symptoms, Process, Treatment and After Care
Meth detox is the process of eliminating methamphetamine from the body while managing withdrawal symptoms. According to “Methamphetamine Withdrawal and Detox” by the American Addiction Centers (2023), the detoxification process is crucial to address both the physical dependence and the brain’s adaptation to the drug. Symptoms of meth detox include fatigue, depression, anxiety, and intense […]
Reward System: Function, Role in Addiction, Addiction Impact, and Genetical Factor

The reward system is a group of neural structures responsible for processing rewarding and pleasurable stimuli. The role of the reward system in drug addiction involves drugs and addictive behaviors that over-activate the reward system, precipitating compulsive “wanting” and seeking of the rewarding stimulus. Repeated drug use causes neuroadaptations that dysregulate the reward system, reducing […]
Quartz Hill California Addiction Statistics

Marijuana Addiction Stats for California: Marijuana use has been a prevalent issue in California for decades, even before its legalization for recreational use in 2018. Here are some key statistics related to marijuana addiction in California that you need to know. Key Takeaways: Adult Marijuana Use in California Here are some statistics on Adult marijuana […]
Xanax Addiction: Meaning, Symptoms, Causes, Effects, and Treatment

Xanax addiction is the uncontrollable urge to use Xanax despite its negative impact. Xanax is a prescription drug for treating anxiety and panic disorders. According to Cardona-Acosta, A. M.’s 2025 study, ‘Mother’s little helper turned a foe: Alprazolam use, misuse, and abuse, ’ alprazolam (Xanax®) is among the most prescribed and abused anxiolytics in the […]
Percocet Addiction: Signs, Causes, Effects, and Treatment

Percocet addiction involves a compulsive reliance on the prescription medication Percocet, which combines acetaminophen for pain relief. This addiction manifests through an overwhelming need to obtain and use the drug, often leading to harmful physical, psychological, and social consequences. Opioids like oxycodone work by binding to specific receptors in the brain and spinal cord, reducing […]
